How to keep muscle cramps from ruining your workouts and competitions
/A CASE STUDY
The scene: It’s a hot, 75 degree Saturday in June, humidity 85%, birds singing. Maybe the most hot and humid day so far this month.
The athlete: Is 6 miles into what is expected to be a 15-mile long run. Last night they enjoyed a couple beers with dinner after completing a 4-mile easy run. Work was pretty hectic, so they drank coffee all day to keep focused. They didn’t consume much water or other fluids.
The cramp: Comes quickly into one calf during the long run, rendering the leg nearly useless and painful, despite the individual believing they weren’t putting out much effort. This has happened before. The runner stretches the muscle for 10 seconds, decreasing the pain and begins to run again. Four minutes later it happens again so they repeat the process until 8 miles, when they finally quit the run out of frustration.
Talk about a wasted training day. Did this runner do something wrong in their preparation for this run? Yes. No. Maybe. Perhaps I’m trying to trick you a little because the truth is we don’t have enough information about the entire situation. What is their maintenance routine like outside of running? Do they strength train? Have they eaten during the initial part of the run?
SO MUCH TO THINK ABOUT
You should see that there are a variety of factors to consider regarding the onset of muscle cramps. Here are some you’ve heard of and maybe some you haven’t:
Prior training experience regarding intensities and durations
History of muscle cramping
Current hydration status, particularly related to level of sweat loss
Electrolyte levels of magnesium, calcium, sodium, and potassium in the blood and muscles
Muscle tone, which is controlled by the nervous system and reinforced by day-to-day use patterns (and also changed with routine soft-tissue maintenance)
Central nervous system status, as in higher anxiety and stress levels
Peripheral nervous system status
Stimulant intake, such as caffeine, which impacts nervous system function
Recent physical activity and fatigue levels
Environmental conditions regarding temperature, humidity, and terrain
Muscular demands at that moment, as in the force of muscle contraction required
Direct muscle trauma
There is likely an interplay of these factors and you therefore need to consider them all in muscle cramp prevention. How are you going to do that? Partly with good regular maintenance and training habits. Partly with a little trial-and-error testing.
Muscle cramps have been a thorn in the side of many athletes for decades, and what fixes them in one athlete may not work for another. Some athletes just seem more prone to cramping while others have minimal issues. I would be surprised if the crowd that is prone to cramping didn’t have at least one or two of these areas to address though.
Available research indicates three main theories exist in the cause of exercise-induced muscle cramping:
“Skeletal muscle overload and fatigue from overuse or insufficient conditioning can prompt muscle cramping locally in the overworked muscle fibers.” (Bergeron, 2008)
“Extensive sweating and a consequent significant whole-body exchangeable sodium deficit can lead to more widespread muscle cramping, even when there is minimal or no muscle overload and fatigue.” (Bergeron, 2008)
“Either neural activity in the spinal cord or in the peripheral could be the cause of the cramps.” (Nakagawa, 2013)
WHAT WE'VE GOT HERE IS A FAILURE TO COMMUNICATE
Lately, the neurological cause has been winning research arguments, so it would make sense to try the solutions that have the most bearing in that area. I frequently tell athletes that the muscles only know what they are told by the nervous system. Without a motor nerve supply, muscles are useless masses of floppy meat. Which means that if the communication between the motor nerves and the muscles goes wrong, you will have a failure of the muscle’s normal function.
This nerve-muscle communication is as much about sending signals to a muscle as much as it is about stopping those signals. It is possible that, with repetitive use and fatigue, the signal from the motor nerve to the muscle isn’t stopped as efficiently as it should be and then the muscle insists on maintaining a contracted state, otherwise known as a cramp.
If cramps occur intermittently for you during exercise, the most likely scenario is one or a combination of these factors:
Poor self-maintenance habits of the muscles
Poor nutritional choices
Subpar preparation of the muscles and nervous system for the task at hand
Neglecting to account for environmental demands
YOUR HOMEWORK
Prevent the cramp with proper preparation and regular maintenance:
First and foremost, if you always cramp in the same muscles, I would not be surprised to find that the resting tension in that muscle was elevated compared to muscles where you don’t ever cramp. Cramping muscles are likely to be more tender to firm pressure. Plus, you may be able to tell that those muscles are physically more taut than your other muscles. Your focus needs to be on getting that resting activity to decrease at all times. For that, you are going to routinely and specifically massage that muscle 1-2 minutes every other day with a massage stick, lacrosse ball, or your hands. It should be uncomfortable to work on the irritable tissue. And it’s going to take a month or two of consistent work to keep that muscle more relaxed. If you want it quicker, then my suggestion is to have dry needling to “reset” the nerve-muscle communication.
Strength train the muscles that routinely cramp to increase their fatigue resistance while simultaneously strengthening any other muscles that can assist with the same motion. For example, the calf muscles are effective pushing muscles so be sure to address any strength loss in the other rearward pushing muscles like the gluteus maximus and hamstrings.
Consider the psychological aspect. Cramping has a lot to do with nervous system function. You aren’t going to make the situation any better by increasing anxiety and stress levels. Athletes that struggle with this need to practice techniques that can lower their stress through deep breathing, meditation, yoga, or sports psychology. It’s no surprise that you could train for weeks without cramps but on race day the anxiety increases at your main event, contributing to the mystery cramps.
Expose yourself consistently to any triggering environmental stimuli, like higher heat and increased humidity.
If you are expecting to be in a competition that requires minimal or significant terrain changes then try to duplicate those changes or lack of changes in your training.
Progress gradually and consistently in durations and intensities of prolonged exercise.
It’s easy to suggest staying hydrated. Typical advice. Just keep your urine on the clearer side consistently. Not just the day of or day before longer exercise bouts. Don’t overhydrate because that can carry health consequences as well.
Consistently eat a well-rounded diet. If you start restricting specific foods that carry important nutrients, then you need to ensure you are obtaining a suitable replacement. For instance, by restricting meat you may cut out a large magnesium source. Do your research on what micronutrient requirements frequent exercisers have and adjust accordingly.
Prevent the cramp during activity:
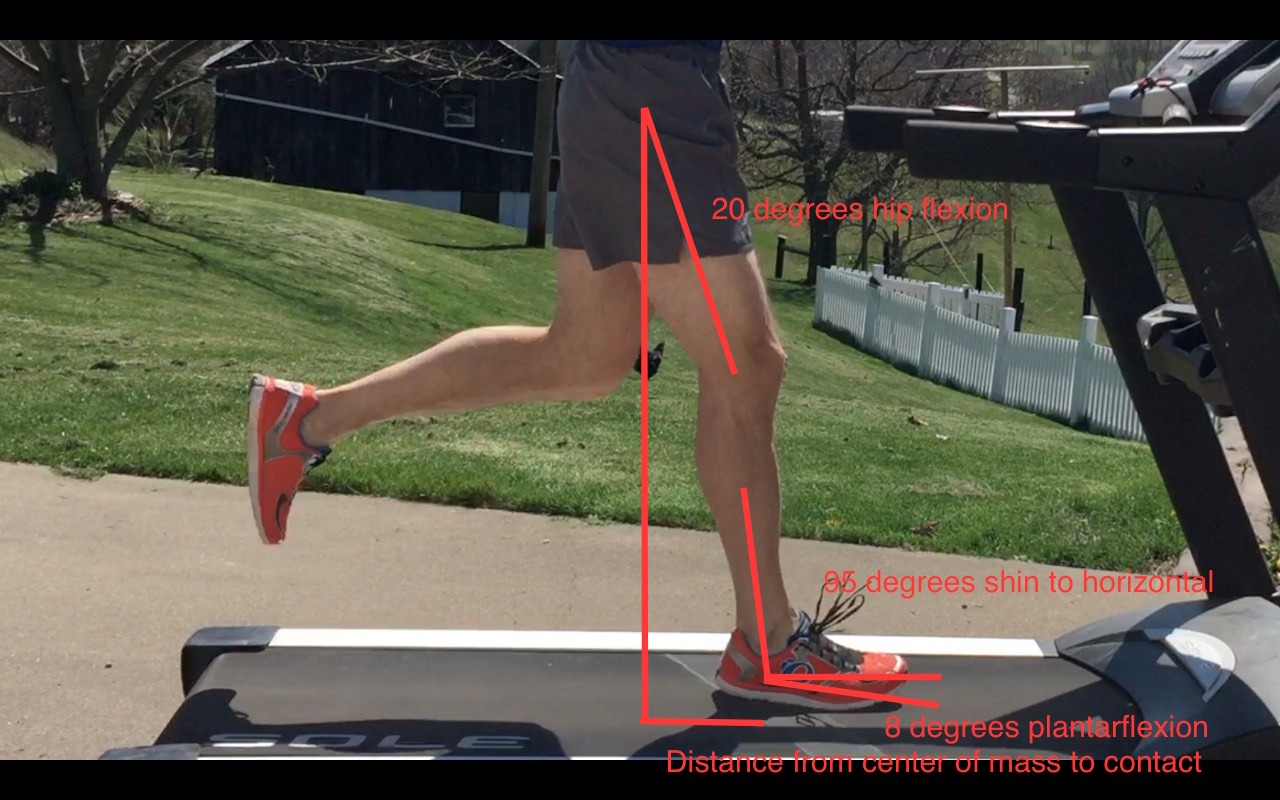
Vary the range of motion and demand on the muscle as much as you can before you have any sense of cramping. For instance, to change the motion and demands of the calf while running switch from your usual forefoot strike to a heel strike for 20-30 seconds every 1-2 miles. Research indicates that the muscle fibers must achieve a shortened state in order to cramp (Bertolasi, 1993). For instance, if you are constantly running on your forefoot, the calf muscle fibers don’t get a chance to elongate, keeping them in a shorter, and riskier, position at all times.
Eat something containing carbohydrates during the exercise. It stands to reason that if muscle fatigue is delayed by eating to supplement energy stores, then you may not cramp as soon or maybe even at all if a few calories are always coming in (Jung, 2005). Nerves must have a supply of energy to function, too. They like glucose. It never ceases to amaze me how many people think they can go harder and faster in an event than they do in training with fewer or worse yet, no calories. Multiple systems change function without normal blood sugar levels.
Stick to a reasonable plan. Just because you feel good physically and mentally from resting a couple extra days prior to competition doesn’t mean you should suddenly decide to pursue higher intensities than you have trained for. Even if you don’t cramp, you will probably bonk in a long event, or blow up in a short event.
If the cramp happens:
Attempt to stretch the muscle. Do not stretch it rapidly and do not stretch it as hard as you can. A gentle but prolonged stretch is the best option at this point. Hold the stretch for at least 30 seconds. Now is not the time to bounce to the end point of the stretch because you have special structures in place to cause muscle contraction when that bounce hits its end point.
Massage the muscle with firm pressure. Even a single, prolonged pressure of 30-60 seconds to the muscle may break its cycle of cramping.
Eat. Didn’t I just go over this?
Try my personal favorite solution, dill pickle juice, as the muscle threatens to cramp. It’s not the salt that is effective but the noxious stimuli from the vinegar. A new sports drink named Hot Shot relies on a similar mechanism but it has more of a spicy flavor. Either way, the potent oral stimulation effects nervous system input.
Try a couple electrolyte tablets or maybe a sports drink containing electrolytes. This isn’t supported by research, but a placebo effect is still a possible effect. But will you still have the placebo effect now that I’ve told you it shouldn’t work? Please let me know how that goes. I personally stopped using them.
Overall, you must adjust according to the variety of factors at hand. If you know you are under-hydrated, aren’t eating enough, haven’t maintained your frequently cramping muscles, undertrained, stressed out, and it’s really humid outside, then your best option is to slow down a little, learn a lesson, and work on the flaws before your next event.
There are instances where cramping with great frequency can be a sign of diseases and serious neurological issues so do not hesitate to contact a medical professional if muscle cramping is occurring outside the realm of exercise. Even a history of sciatic nerve problems can predispose a person to cramping during exercise.
Take care of the muscles and the nervous system with planning and preparation and they will take care of you.
Please let me know if you have any questions at derek@mountainridgept.com. And definitely let me know if you find some of these ideas helpful in muscle cramp management by liking the Mountain Ridge Physical Therapy Facebook page. Or buy me some dill pickles.
For those who would like to geek out on some related material:
http://journals.lww.com/acsm-csmr/Abstract/2008/07001/Muscle_Cramps_during_Exercise_Is_It_Fatigue_or.9.aspx
http://link.springer.com/article/10.2165/00007256-199621060-00003#page-1
https://www.researchgate.net/publication/299960193_Neural_Mechanisms_of_Muscle_Cramp
http://home.trainingpeaks.com/blog/article/controlling-neuromuscular-performance-to-prevent-muscle-cramps?utm_source=tpr&utm_medium=email&utm_campaign=07-16-anl